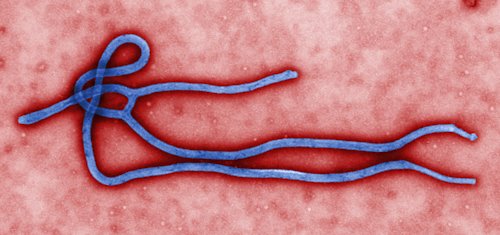
The focus of the media may not have strayed far from the same core issues over the past few weeks and months, from the conflicts in Syria and Iraq to Russia's involvement in Ukraine, not to mention the Scottish Independence Referendum, but a steady stream of grounding images documenting the spread of Ebola through West Africa has played an almost constant second fiddle.
The biggest Ebola outbreak on record is spreading fast through the west of the continent, with Liberia, Sierra Leone, Guinea and Nigeria affected. An estimated 3,000 people have now fallen victim to the disease, and the World Health Organisation (WHO) has declared it an international health emergency.
Interestingly, a small number of reports have looked beyond the horror of the suffering to the reality of what happens next. Ebola is transmitted via bodily fluids, making dealing with the dead particularly perilous.
In many of the affected countries, the government-led 'burial teams' on the ground are faced with daily dangers of hostile mobs in addition to the obvious risks of transmitting the disease.
Some bereaved families refuse to accept Ebola as a cause of death for fear of persecution in their local towns and villages. Those tarred with the Ebola brush are cast out, with some communities convinced that the ghastly symptoms reflect evil spirits at work; not a viral disease.
This renders the work of the countries' burial teams riskier still, with those in Liberia rarely spotted without a police escort in tow following a series of violent attacks.
Clad head to toe in white, the teams' masks, gloves and boiler suits, vigorously taped at the wrists to ensure nothing passes this protective barrier, present an unmistakable sight now synonymous with Ebola. The process they follow echoes their sterile appearance and is inherently clinical in nature; any cultural or religious practices involving physical contact between the family and the deceased are forbidden, much to the great upset of many who have lost a loved one.
First, the burial team will disinfect the body several times over before sealing it twice in plastic shrouds to prevent any residual infectious fluids from escaping. What happens next will vary; the policies differ depending on the affected nation's policy. Some are transported to a specified area for the burial of Ebola victims, while others are cremated. Any pillows, bed sheets or clothing which have come into contact with the body, as well as the workers' protective gear, are then buried or burnt along with the body in an attempt to minimise any risks of passing on the infection.
In either case, the likelihood of confirming whether or not the deceased was, in fact, a victim of Ebola is minimal. In the haste to deal with the body so as to limit transmission of the disease, testing is often not carried out, meaning some families and communities are wrongly labelled as Ebola zones.
While the WHO has voiced concerns that those on the ground in the affected West African nations aren't sufficiently equipped to deal with these highly infectious bodies safely, the Red Cross has praised the work of officials in Sierra Leone where a set process carried out by specialised "dead body management teams" has been implemented with much success.
These brave individuals who are risking their lives to look after victims of Ebola may be just the key to stopping the deadly disease in its tracks.